Traumatic neuromas are infrequent benign tumors that frequently develop after trauma or surgery and are characterized by painful symptoms that are easy to identify. In clinical practice, traumatic neuromas are extremely uncommon, however, they are relatively common after a traumatic event or surgery. Pain and paresthesia are the predominant clinical symptoms. Researchers agree that traumatic neuromas are benign tumors since their development is linked to abnormal or excessive hyperplasia following nerve damage.
Definition
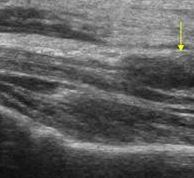
A traumatic neuroma is a mass of entangled nerve fibers and connective tissue that forms when a nerve is damaged. Typically, it appears as a 2 cm or smaller solid, oval, whitish, painful nodule that is slowly expanding. Paresthesia over the wounded area could also be present.
Symptoms
Depending on the site of the damage and its intensity, traumatic neuroma symptoms may include:
- The most common symptom is pain, which can be mild or severe, constant or intermittent, and throbbing or aching.
- The discomfort, which is frequently characterized as "burning," "tingling," or "pins and needles," may be worse at night or during colder months.
- Sensory problems may include tingling, numbness, or a "crawling" feeling in the region supplied by the damaged nerve.
- Damage to a nerve can cause motor problems such as weakness and atrophy in the area supplied by that nerve.
- Allodynia is a condition in which a person feels pain from things that ordinarily would not hurt them, including a light touch or a gentle breeze.
- Hyperalgesia is a condition in which a person has an enhanced sensitivity to the sensation of pain that they are experiencing.
Causes
Peripheral nerve damage results in traumatic neuromas. An accident, a local anesthetic injection, or a surgical operation, such as tooth extraction, may cause damage to the mouth cavity. An injured sensory nerve may become transected, which can cause swelling and scarring. As the proximal nerve portion attempts to regrow into the distal nerve portion, it becomes entangled and stuck in the forming scar, resulting in a disordered mass of fibrous tissue, Schwann cells, and axons.
Pain is seen in almost half of the individuals with oral traumatic neuromas. Pain can range from occasional sensitivity to chronic, severe discomfort. Traumatic neuromas can occasionally produce radiating face pain. The discomfort is reduced by administering a local anesthetic to the tumescent region.
Treatment
The damaged nerve is often surgically removed as part of treatment for a traumatic neuroma. This can be accomplished by more conventional open surgery or through less intrusive techniques such as endoscopic surgery. Both methods are viable options. It is possible that a recommendation for physical therapy will be made to aid in the rehabilitation process and stop the formation of compensatory movement patterns. The management of discomfort and pain in some circumstances may involve the use of drugs or pain-relieving procedures like nerve blocks. Alternative treatments, such as injectable therapy or nerve decompression, may be considered in certain circumstances where surgical excision of the tumor is either not possible or not the best course of action.









0 Comments
For comments please reply here.......